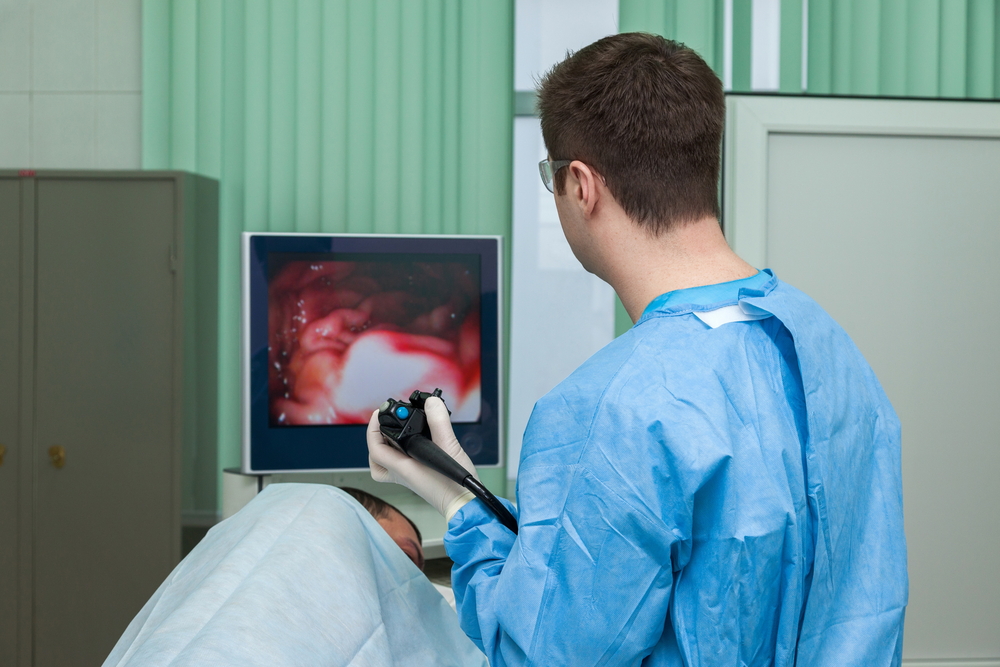
 Researchers at the University of Buffalo are developing an endoscope that has the capacity to zap tumors and lead to chemotherapy improvements, reducing its toxic side effects and improving the capacity to treat some forms of malignant cancers.
Researchers at the University of Buffalo are developing an endoscope that has the capacity to zap tumors and lead to chemotherapy improvements, reducing its toxic side effects and improving the capacity to treat some forms of malignant cancers.
This innovative system will be particularly helpful in the treatment of lung cancer, along with ovarian cancer with abdomen metastasis and gastrointestinal tract cancer.
Doctors commonly use an endoscope, a small tube with an incorporated light and camera at the tip, to examine internal organs, aiding in cancer and other malignancies’ detection. However, the established endoscoping imaging techniques have their limitations, including a distorted image contrast due to absorbed light by the patient’s own body, leading to low-contrast images of the area surrounding the tumor, blocking the doctor’s capacity to correctly visualize it.
“We are developing a novel endoscopic device that will improve our ability to detect and destroy cancer cells,” principal investigator Ulas Sunar, PhD, a research assistant professor in UB’s Department of Biomedical Engineering said in a news release.
In an attempt to resolve these problems, the investigational endoscope has the capacity to use spatial frequency domain imaging, a novel technique that can correct the image contrast through light pattern projection of different frequencies on cancer cells, resulting in a high-contrast map of the cancer microenvironment.
“We expect doctors in the operating room will greatly benefit from this device,” Dr. Sunar added.
To efficiently zap the tumors, chemotherapy drugs will be delivered intravenously using small liposomes as delivery vehicles (nanoballons). This experimental technology is being developed by Jonathan Lovell, PhD, UB assistant professor of biomedical engineering, and can carry drugs directly towards tumor cells while at the same time protecting healthy cells from direct contact with the drugs, reducing possible toxic side effects.
When the nanoballons reach their targets, doctors can use the endoscopic light beam to rupture these structures, allowing the drug to spread directly onto the tumor.
Dr. Sunar’s laboratory is developing a digital mask that can efficiently target the nanoballoons, adjusting the beam’s intensity and manipulating its shape.
“The mask is sort of like the Bat signal from Batman movies. It alters the shape of the light,” explained Dr. Sunar. “At the same time, we’ll be able to control the strength of the light. The combination will allow us to manipulate the beam to target cancer cells with unprecedented accuracy.”