 Research conducted in the laboratory of Kenji Suzuki, MD, at Juntendo University School of Medicine in Tokyo, is helping to increase the prognostic power for lung cancer. In an article published in The Annals of Thoracic Surgery, the research team explained how visceral pleural invasion (VPI) can predict survival of patients with small solid lung tumors but not part-solid tumors.
Research conducted in the laboratory of Kenji Suzuki, MD, at Juntendo University School of Medicine in Tokyo, is helping to increase the prognostic power for lung cancer. In an article published in The Annals of Thoracic Surgery, the research team explained how visceral pleural invasion (VPI) can predict survival of patients with small solid lung tumors but not part-solid tumors.
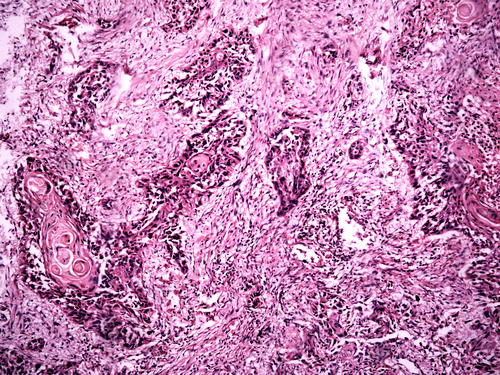
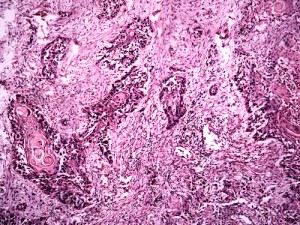
According to an unrelated article published in The Journal of Thoracic Cardiovascular Surgery, “VPI is defined as [tumor cell] invasion beyond the elastic layer, including invasion to the visceral pleural surface.” It is the topic of a number of studies investigating its prognostic power for non-small-cell lung cancer (NSCLC), a severe form of lung cancer.
Despite its utility as an indicator of adverse prognosis for NSCLC, VPI had been unexplored in tumors with ground-glass opacity lesions, including tumors that appear part-solid, due to this tumor type’s minimally invasive nature. To mitigate the lack of knowledge, Dr. Suzuki’s team used thin-section computed tomography (CT) to scan 446 patients with surgically resected, node-negative part-solid or pure-solid NSCLC and compared the five-year survival rates to the appearance of the tumors.
All tumors were less than 30 mm in size, and part-solid nodule appearance was defined as having both a solid and ground-glass opacity. To be considered a pure-solid nodule, tumors needed to show consolidation without ground-glass opacity.
In total, 10% of patients with part-solid nodules and 38% of patients with pure-solid nodules had VPI. Only patients with pure solid-nodules could have 5-year survival predicted by VPI: five-year survival rate was worse in patients with VPI than that of patients without VPI (70.1% versus 81.3%). In contrast, five-year survival rates for part-solid nodule patients with and without VPI were 85.6% and 94.9%, respectively, showing no significant relationship.
The study is important because VPI “increases the T staging factor from T1 to T2 and upstages a tumor from stage IA to stage IB pathologically.” T staging factor is an assessment of primary tumors among assessments for regional lymph nodes and distant metastatic sites in the American Joint Committee on Cancer’s and the International Union for Cancer Control’s TNM system. This change in stage may sway a clinician to administer adjuvant chemotherapy to a combat patient’s lung cancer, a decision that must be made with great care.